A meta-analysis indicates that 25% of patients with PD with normal cognition progressed to PD with MCI (PD-MCI), and 20% of PD-MCI progressed to PDD within 3 years ( Saredakis et al., 2019). Mild cognitive impairment (MCI) may be a precursor of PDD ( Goldman and Sieg, 2020) and is common in PD patients without dementia (mean cross-sectional prevalence, 26.7% range, 18.9–38.2%) ( Litvan et al., 2011), and can be present in patients with early-stage PD. A systematic review yielded a PD patient with dementia (PDD) point prevalence of 31.3% ( Aarsland and Kurz, 2010), and the cumulative prevalence from 8 years of follow-up found that up to 78% of PD patients eventually developed PDD ( Aarsland et al., 2003). 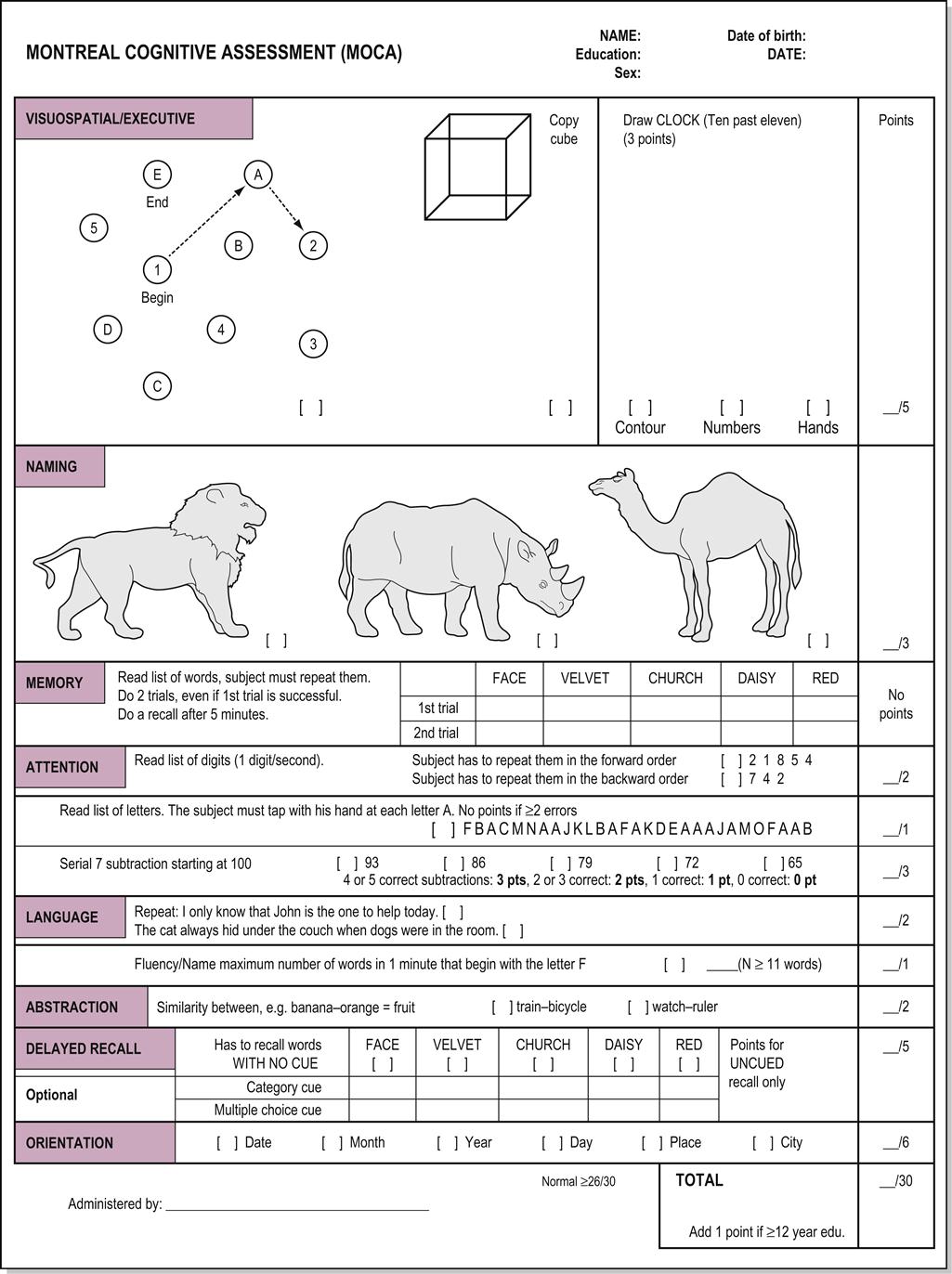
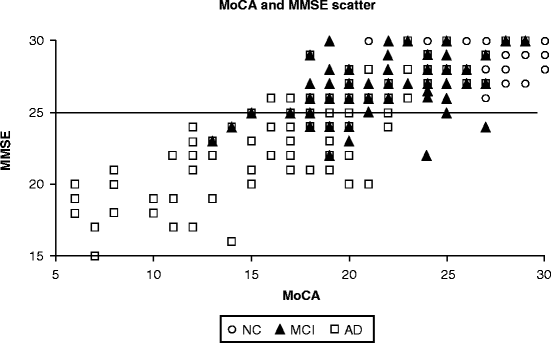
Cognitive dysfunction may affect how patients effectively deal with real-life problems, emphasizing an individual’s function ( Anderson et al., 2013). Motor symptoms are the predominant clinical manifestation of PD, but non-motor symptoms are also prevalent ( Liu et al., 2015 Schapira et al., 2017), such as cognitive dysfunction ( Yu et al., 2010, 2012a, 2015b), social brain dysfunction ( Yu et al., 2012b, 2018 Yu and Wu, 2013a), and sleep disturbances ( Yu et al., 2015a). Recent global data indicate that the prevalence of PD in ages 40–49 is 41 per 100,000 individuals and up to 1903 per 100,000 individuals among those over the age of 80 years ( Pringsheim et al., 2014). The number of individuals diagnosed with PD has grown significantly in the past three decades worldwide ( Armstrong and Okun, 2020). Parkinson’s disease (PD) is a chronic, progressive neurodegenerative disorder. The AUCs of the two tests were 0.846 ( p < 0.001) and 0.794 ( p = 0.003).Ĭonclusion: We suggest considering both cognitive and social functions when detecting PD-MCI and PDD. When the simplified MoCA was 7 or the combined test 30, the patients would be classified as having PDD. The discrimination values measured by the area under the receiver operating characteristic curve (AUC) of the two tests were 0.767 ( p < 0.001) and 0.790 ( p < 0.001). Results: To detect PD-MCI, the optimal cut-off scores for the simplified MoCA and the combined test were 9 and 35. According to the MDS diagnostic criteria, the patients were grouped into PD-nonMCI, PD-MCI, or PDD. Materials and Methods: A total of 166 participants (84 PD patients and 82 healthy) were recruited who completed the MMSE, MoCA, PD social functioning scale (PDSFS), clock drawing test, activities of daily living, comprehensive neuropsychological assessment (e.g., executive, attention, language, memory, and visuospatial functions), and movement disorder society (MDS)-unified PD rating scale. Objective: We aimed to simplify the commonly used tools and combine cognitive and social functioning tests to detect early MCI and PDD. A composite assessment that considers both cognitive and social dysfunction in PD would be helpful in detecting mild cognitive impairment (MCI) and PD dementia (PDD). 4Department of Neurology, National Cheng Kung University Hospital, College of Medicine, National Cheng Kung University, Tainan City, Taiwanīackground: The commonly used screening tests for Parkinson’s disease (PD) are the Montreal Cognitive Assessment (MoCA) and Mini-Mental State Examination (MMSE), both of which only focus on cognitive function.3Graduate Institute of Clinical Medicine, College of Medicine, Kaohsiung Medical University, Kaohsiung City, Taiwan.2Department of Neurology, Kaohsiung Medical University Hospital, Kaohsiung Medical University, Kaohsiung City, Taiwan.1Institute of Behavioral Medicine, College of Medicine, National Cheng Kung University, Tainan City, Taiwan.Ya-Wen Yu 1 Chun-Hsiang Tan 2,3 Hui-Chen Su 4 Chung-Yao Chien 4 Pi-Shan Sung 4 Tien-Yu Lin 4 Tsung-Lin Lee 4 Rwei-Ling Yu 1* 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
